Sudan Media Forum
Khartoum, April 8, 2026 (Ayin Network) – On April 7, as the world marks World Health Day under banners of well-being and medical advancement, Sudanese people awaken to a reality stripped of even the most basic conditions for survival. The conflict between the Sudanese Armed Forces and the Rapid Support Forces has evolved into a silent war waged within exhausted bodies and spirits drained by relentless strain.
In the Al-Droshab neighborhood of Khartoum North, “Ahmed” lives with his extended family in a single home, where daily life has become a quiet battle against hunger, illness, and soaring medical costs. Speaking to Ayin, Ahmed—a father of two—describes how the family’s diet has drastically changed since the war began. Meals are no longer the same in quantity or quality.
“Before the war, we were managing. The children ate three meals a day, with fruit and milk. Now we’re down to two meals, and even the type of food has changed… we rely on whatever just fills the stomach.”
Daily Life Under the Weight of Hunger

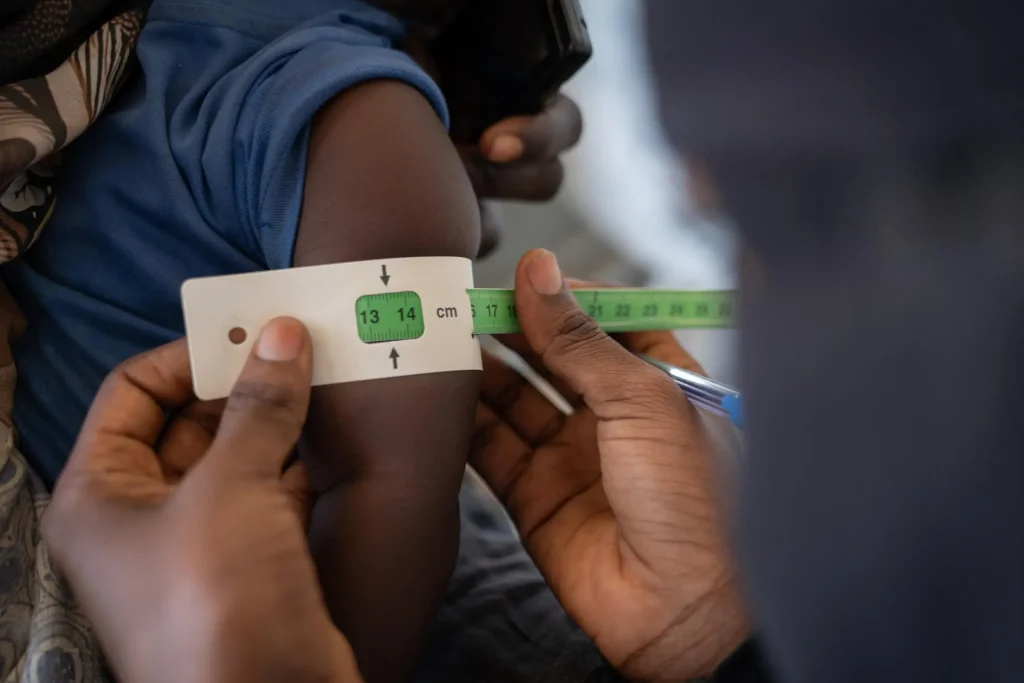
Ahmed’s account reflects a catastrophic reality confirmed by international reports: food insecurity in Sudan has reached “catastrophic” levels, with 21.2 million people facing acute hunger. This decline is not merely about feeling hungry—it is a direct driver of mortality. Ahmed links his children’s weakened immunity to poor nutrition, noting they can no longer fend off illness as they once did.
The crisis is even more visible in displacement areas. In July 2025, the Integrated Food Security Phase Classification (IPC) Famine Review Committee confirmed famine conditions (Phase 5) in Zamzam camp in North Darfur. In areas such as Um Baru and Karnoy, global acute malnutrition (GAM) rates exceeded 53%—far beyond emergency thresholds.
This deterioration in food quality has directly affected Ahmed’s children, who now fall ill frequently. He attributes their vulnerability to weakened immunity caused by poor nutrition, compounded by deteriorating living conditions marked by the spread of insects and declining sanitation.
At the same time, accessing healthcare has become increasingly complex. Beyond limited availability, the cost of treatment imposes harsh choices between health and survival. Ahmed recalls a recent incident when one of his children fell ill, forcing him to pay an amount equivalent to a full month’s household expenses for consultation and medication.
“The real pain is having to choose between treating your child and feeding the rest of the family,” he says.
The hardship extends beyond children. Ahmed’s father suffers from a chronic condition requiring regular medication unavailable locally, forcing the family to rely on supplies sent from relatives abroad.
Ahmed’s story mirrors a broader crisis, where economic pressures intersect with the collapse of the healthcare system, creating a reality he describes simply: survival has become a complex equation between affording treatment and enduring daily life—an equation that increasingly burdens mental health.
From Shock to Long-Term Psychological Depletion
“Dr. Khalid”—a pseudonym for a psychiatrist—tells Ayin that what Sudanese society is experiencing is no longer a conventional health crisis but a profound fragmentation of collective psychological structure. He describes a transition from initial “shock” to a state of long-term psychological depletion, where individuals live under continuous pressure beyond the nervous system’s capacity to endure.
Prolonged exposure to daily danger has created a condition of “constant alertness,” placing people in a permanent defensive mode and leading to gradual emotional and psychological exhaustion.
“People are no longer responding to life naturally. They operate almost mechanically just to get through the day… simply trying to survive.”
According to his analysis, the impact extends beyond the current generation, threatening future generations through what is known as trauma transmission. Fear and mistrust risk becoming embedded in children’s psychological makeup, undermining future social cohesion.
Dr. Khalid notes that children and women are particularly vulnerable, especially amid disrupted education and the absence of safe environments. Children lose the sense of stability that schools provide, while women—especially survivors of violence—face compounded trauma in the absence of adequate psychosocial support services.
He also highlights the psychological toll of displacement and loss of home. In the Sudanese context, losing one’s home means losing both safety and identity, leaving deep scars on dignity and stability—especially among the elderly, whose lives are closely tied to familiar environments.
Despite the bleak outlook, he points to emerging community and digital initiatives attempting to fill gaps in mental health support by providing safe spaces for expression and solidarity. However, he stresses that these efforts remain limited unless mental health is systematically integrated into the broader healthcare system through community training and expanded services.
Healthcare workers themselves, he adds, are under immense psychological strain, operating in a collapsed system with minimal resources—leading to emotional burnout and affecting the quality of care.
“The doctor here is treating others while carrying the same wounds… trying to save lives while fighting a personal battle for survival.”
He concludes by emphasizing that Sudan’s challenge is not only rebuilding infrastructure but addressing the deep psychological consequences of war—starting with acknowledging the scale of trauma and moving toward a human-centered response model.
Working Under Continuous Crisis
From a medical laboratory in Omdurman, “Dr. Sara” describes her work as operating under constant pressure. Despite mounting challenges, medical staff strive to maintain minimum diagnostic standards. She notes that the lab continues to function at full capacity, focusing on tests related to widespread diseases such as malaria and dengue fever, alongside chronic conditions like thyroid disorders and diabetes.
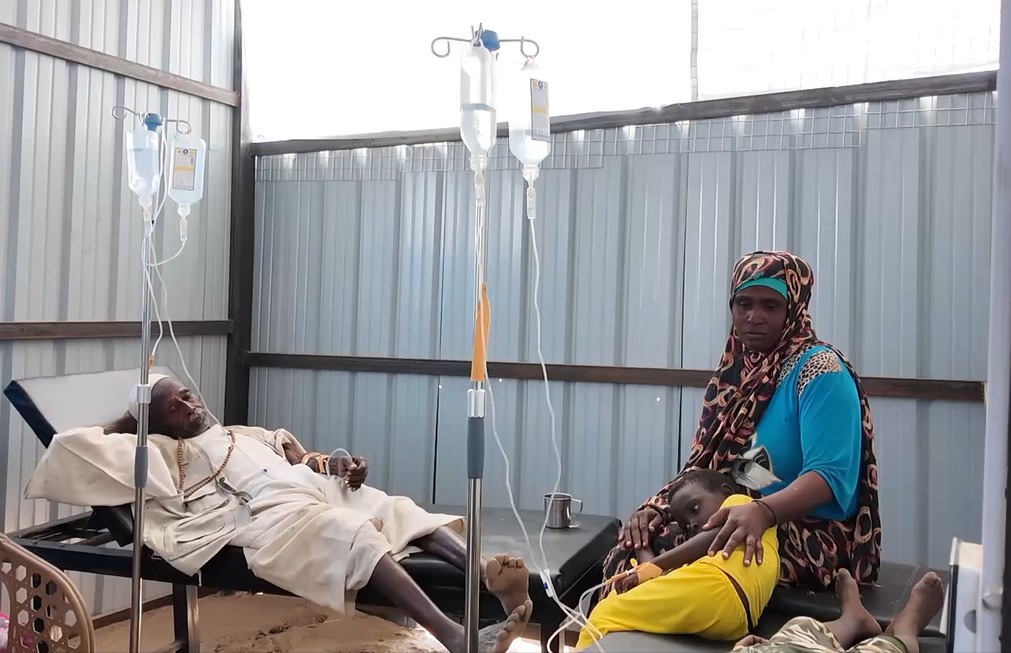
However, supply stability remains uncertain, as laboratories depend on shipments from cities such as Atbara and Port Sudan, making the availability of certain tests inconsistent.
In the absence of reliable diagnostics, physicians often resort to clinical judgment and symptom-based treatment. While sometimes effective, Dr. Sara acknowledges that this approach is a forced compromise rather than an ideal solution.
“We are working within continuous crises,” says “Dr. Samer,” summarizing the reality of Sudan’s healthcare sector in conflict zones.
He explains that what remains of healthcare facilities no longer operates as an integrated system, but rather as “points of resilience” under extreme pressure. The few hospitals still open face overwhelming overcrowding and severe shortages of clean water and electricity—basic requirements for any medical service. In many areas, healthcare is entirely absent.
“At best, we work in hospitals that are unbearably crowded, without clean water or stable electricity… and in other places, there are no hospitals at all.”
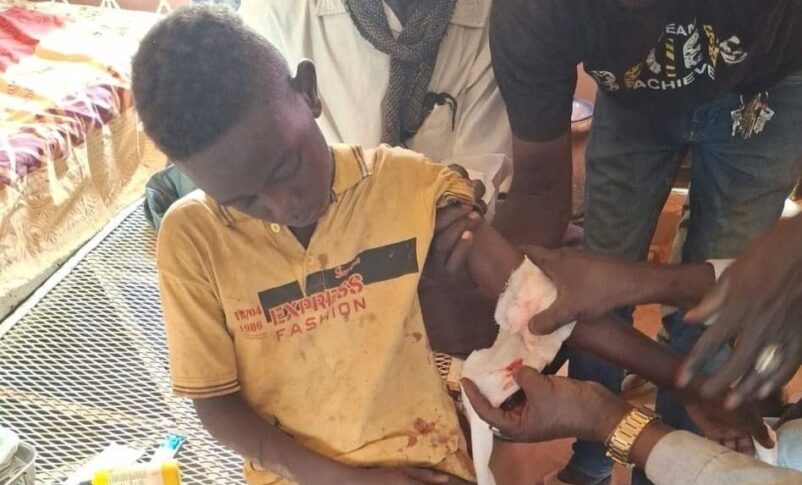
The challenge extends beyond infrastructure to a high-risk working environment. Attacks on healthcare facilities have transformed the profession from humanitarian service into a dangerous occupation.
According to the Sudan Doctors Network, repeated assaults on hospitals and medical personnel have been documented. In East Darfur, forces affiliated with the Rapid Support Forces stormed a family hospital in Al-Daein, assaulting medical staff and completely destroying equipment, halting services.
The same state also witnessed an airstrike targeting Al-Daein Teaching Hospital, killing four people, including children, and injuring three others.
In White Nile State, seven people—including two healthcare workers—were killed when a drone strike hit Al-Jabalain Hospital while doctors were on duty.
These incidents, the network notes, reflect a recurring pattern of targeting healthcare facilities by parties to the conflict. This aligns with Dr. Samer’s testimony that “hospitals are no longer safe spaces—they have become potential targets.”
“The danger doesn’t only come from shelling or clashes,” he adds. “It extends to security persecution.” He recounts his own arrest on accusations of “collaborating with one of the conflict parties”—a charge increasingly used against medical workers simply for treating the wounded.
Though later released following community intervention, he describes the experience as a turning point that exposed the fragility of protections supposedly afforded to healthcare workers.
The Sudan Media Forum and its member organizations publish this report, prepared by Ayin Network, on the occasion of World Health Day. It documents the dire state of Sudan’s healthcare sector amid the ongoing war between the Sudanese Armed Forces and the Rapid Support Forces.
The report details repeated attacks on hospitals and medical personnel, including drone strikes and arrests, as part of a broader systemic collapse rendering the healthcare system extremely fragile. As one doctor puts it: “What Sudanese society is experiencing today is no longer a conventional health crisis—it is a profound disintegration of the collective psychological structure.”




